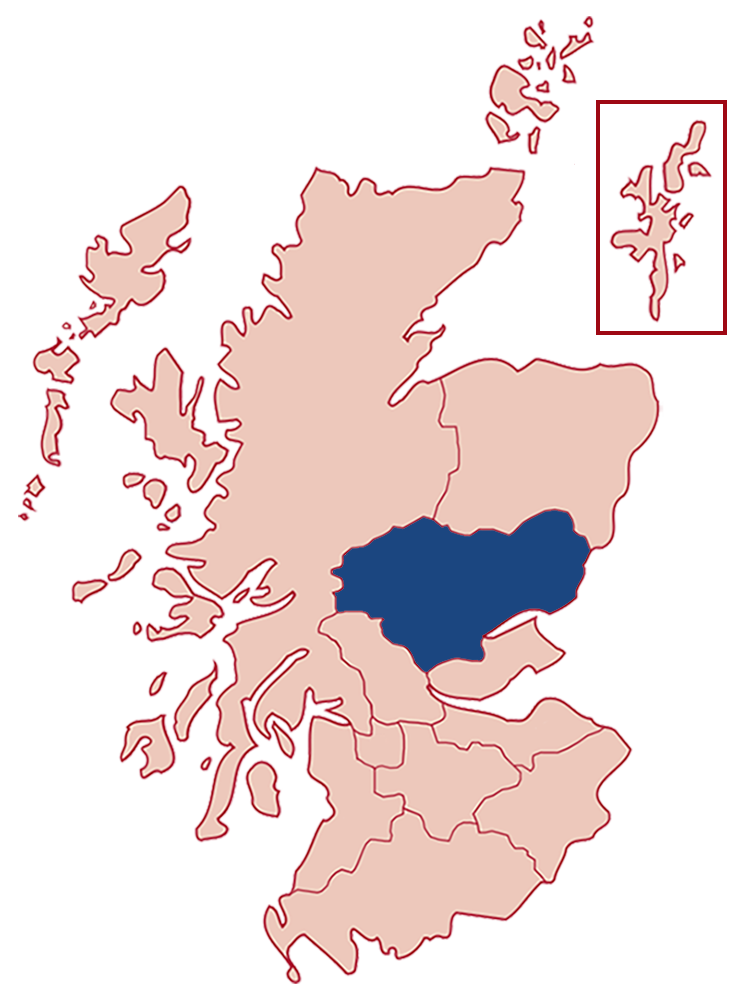
Tayside
Patients per year
549
from 515 in 2012.
Urban / rural split
76%
from 76% in 2012.
Total region population
415,470
from 402,641 in 2012.
Specialist HF nurse WTE posts
3 WTE (3 staff)
from 3 WTE, from 3 staff in 2012.
Service provision
| 2012 | 2018 |
|---|---|
| HFrEF | HFrEF |
| HFpEF | HFpEF |
| HF post MI | HF post MI |
| Valvular HF | Valvular HF (only with LVSD) |
| Congenital HF | Congenital HF |
| Palliative Care | General palliative care and pathway to specialist services |
| Cardiac Rehabilitation for HF | |
| Screening for psychological distress- direct referrals to psychology |
Service model
| 2012 | 2018 |
|---|---|
| Home | Home |
| Clinic | Clinic |
| In-pt education | In-pt education |
| In-pt management | In-pt management |
| GP surgery | GP surgery |
| Virtual | Virtual |
Additional notes
Service achievements
- Clinic system developed
- Heart Failure nurse delivery of psychological assessment (Heart Failure Hub support)
- Participation in the national Palliative Care Programme (Heart Failure Hub support)
- Improved coding on discharge (use of 5th digit identifying those with LVSD)
- BNP in use to triage/streamline echo requests and fast track clinical input as appropriate.
- MDT established.
Service challenges
- Increased patient numbers and complexity, resulting in longer time within the service.
- Additional patients re-referred to service requiring support for commencing Entresto.
Future improvements
- Implementation of a step down services i.e. virtual and optimisation clinics.
- New database to support cardiology nursing services
REMINDER
The following details are from our 2012 report and may not reflect the current state of the Tayside Health Board.
Further details
| (Actual number of staff) | 2008 - 3 WTE (3 staff) |
| SIGN Ratio | 1:134,214 (2008 1:130,546) |
| Ave. caseload per post | 90 (community) |
| Individual patients managed by service (average year) | 515 patients |
| Service Provision | Home visits 70% / Telephone follow-up 30% |
| Provision for HF-PEF | No |
| Administration support per week | 30 hours (across service) |
| Providing education to non-specialist staff | Yes – variety; ward/primary care, protected learning time events, Dundee University modules. |
| Doctor with specialist interest in Heart Failure | 2 (Clinical Lead for Heart Failure and Heart Failure Specialist Consultant) |
| Cardiac Rehabilitation available/number seen | Yes – 25 patients per annum |
| Access to psychological support referral pathway | None |
Notes on current service provision
Providing home and telephone follow up for patients following discharge from hospital or following clinic review where they have been identified as unstable. This model of delivery supports general heart failure management and rapid response to clinical deterioration, through advancing illness to end of life support. Strong links with the palliative care team provides specialist input and seamless care in the community setting and prevention of readmissions remains a key target.
Funding in comparison to 2008
Core funded by NHS Tayside.
Challenges
Standards for review timelines post discharge are challenging due to both numbers and location and remain under evaluation. The provision of rapid response (in a rural setting), has resulted in improved cross-boundary working and improved liaison across the specialities.
Development opportunities
All three nurses in the team are Independent Prescribers and two have also completed the Palliative Care module (for heart failure) at Glasgow Caledonian University. Recent Royal College of Nursing/Office for Public Management economic analysis of the Tayside service has identified clear financial benefits that may be achieved by organisational investment in the service; this analysis is to be further explored at Cardiology Management level.