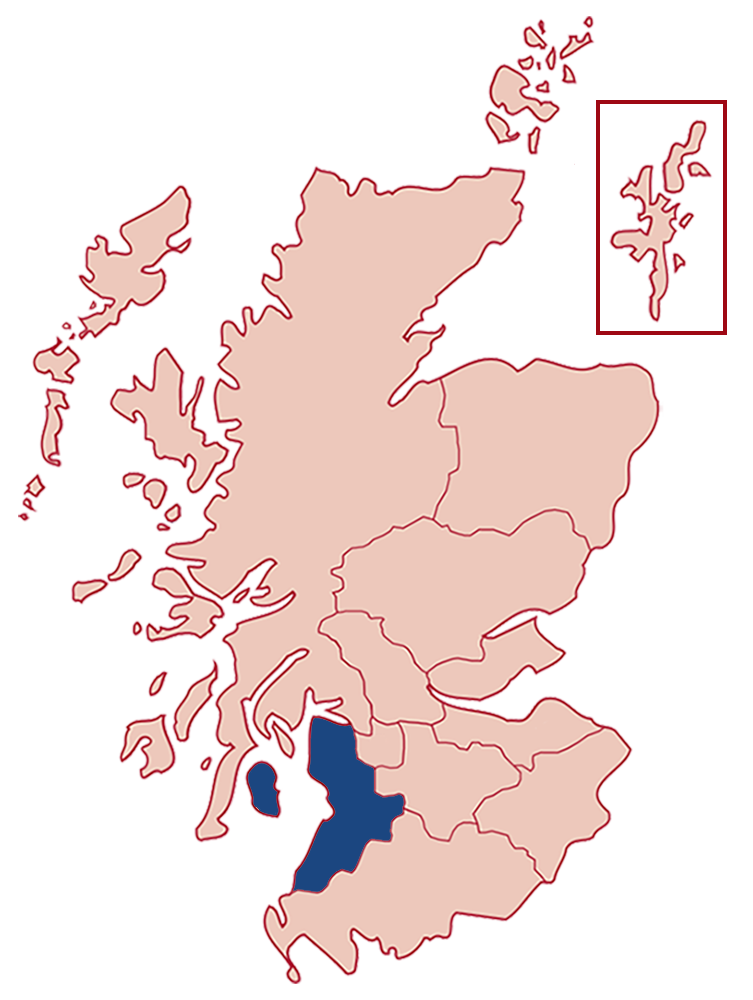
Ayrshire and Arran
Patients per year
482
from 348 in 2012.
Urban / rural split
78%
from 78% in 2012.
Total region population
370,410
from 366,860 in 2012.
Specialist HF nurse WTE posts
5 WTE (4 staff)
from 4 WTE, from 7 staff in 2012.
Service provision
| 2012 | 2018 |
|---|---|
| HFrEF | HFrEF |
| HFpEF | HFpEF |
| HF post MI | HF post MI |
| Valvular HF | Valvular HF (only with LVSD) |
| Congenital HF | Congenital HF |
| Palliative Care | General palliative care with pathway to specialist services |
| Cardiac Rehabilitation for HF | |
| Screening for psychological distress- direct referrals to psychology |
Service model
| 2012 | 2018 |
|---|---|
| Home | Home |
| Clinic | Clinic |
| In-pt education | In-pt education |
| In-pt management | In-pt management |
| GP surgery | GP surgery (stand alone clinics) |
| Virtual | Virtual |
Additional notes
Service achievements since the last review in 2013
- Implementation of home health monitoring.
- New database developed for audit and record keeping
- Development of electronic referral process
- Use of electronic communications e.g. iPad, staff development programme with Cardiac Rehab, out-patient nurse led clinic at both sites.
Service challenges since the last review in 2013
Staffing levels is problematic which reduces the ability of the team to innovate
Future improvements
- Reintroduction of outpatient Intravenous (IV) diuretics
- Exploration of rapid response and early supported discharge services
- Weekly MDT.
REMINDER
The following details are from our 2012 report and may not reflect the current state of the Ayrshire and Arran Health Board.
Further details
| (Actual number of staff) | 2008 * 5 WTE (6 staff) |
| SIGN Ratio | 1:91,715 (2008 1:73,290) |
| Ave. caseload per post | 125 (community) / 225 (hospital) |
| Individual patients managed by service (average year) | 348 patients |
| Service Provision | Home visits 80% / Clinic Appointments 20% |
| Provision for HF-PEF | No |
| Administration support per week | 18.75 hours (across service) |
| Providing education to non-specialist staff | Yes - informal basis to non-specialist staff |
| Doctor with specialist interest in Heart Failure | 1 Consultant Cardiologist (non-specialist) |
| Cardiac Rehabilitation available/number seen | Yes - 80 patients in total |
| Access to psychological support referral pathway | Inadequate (currently recruiting to clinical post) |
Notes on current service provision
Three full-time posts are based in the community to follow-up patients discharged from secondary care and four advanced specialist nurses are based within the acute setting; their posts also cover Chest Pain Assessment, outpatient Rapid Access Chest Pain clinics and Cardiac Rehabilitation. Most referrals are from secondary care, although 30 were also received direct from GPs.
Funding in comparison to 2008
The service is core funded by the NHS with adequate provision, although the previous BHF Post of Palliative Care Specialist Nurse did not receive ongoing funding. The service is undergoing a process of succession planning for the Specialist Nurse posts.
Challenges
The service is facing rising caseloads and differing methods of management are predicted to be challenges for the future. A replacement lead for the established Clinical Psychology service is awaited.
Development opportunities
A new database was recently implemented within the service and the specialist nurses are leading on the implementation of the HF Bundle across the NHS Board. New projects currently include tele-monitoring and the administration of diuretics (through a BHF funded secondment for 2 years). A new ICD pathway is also in the process of being implemented which will have the potential to impact on patients and the service.